85 results
Preeclampsia and risk of maternal pulmonary hypertension at high altitude in Bolivia
- C. E. Salinas, O. V. Patey, C. Murillo, M. Gonzales, V. Espinoza, S. Mendoza, R. Ruiz, R. Vargas, Y. Perez, J. Montaño, L. Toledo-Jaldin, A. Badner, J. Jimenez, J. Peñaranda, C. Romero, M. Aguilar, L. Riveros, I. Arana, D. A. Giussani
-
- Journal:
- Journal of Developmental Origins of Health and Disease / Volume 14 / Issue 4 / August 2023
- Published online by Cambridge University Press:
- 27 July 2023, pp. 523-531
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Women with a history of preeclampsia (PE) have a greater risk of pulmonary arterial hypertension (PAH). In turn, pregnancy at high altitude is a risk factor for PE. However, whether women who develop PE during highland pregnancy are at risk of PAH before and after birth has not been investigated. We tested the hypothesis that during highland pregnancy, women who develop PE are at greater risk of PAH compared to women undergoing healthy highland pregnancies. The study was on 140 women in La Paz, Bolivia (3640m). Women undergoing healthy highland pregnancy were controls (C, n = 70; 29 ± 3.3 years old, mean±SD). Women diagnosed with PE were the experimental group (PE, n = 70, 31 ± 2 years old). Conventional (B- and M-mode, PW Doppler) and modern (pulsed wave tissue Doppler imaging) ultrasound were applied for cardiovascular íííassessment. Spirometry determined maternal lung function. Assessments occurred at 35 ± 4 weeks of pregnancy and 6 ± 0.3 weeks after birth. Relative to highland controls, highland PE women had enlarged right ventricular (RV) and right atrial chamber sizes, greater pulmonary artery dimensions and increased estimated RV contractility, pulmonary artery pressure and pulmonary vascular resistance. Highland PE women had lower values for peripheral oxygen saturation, forced expiratory flow and the bronchial permeability index. Differences remained 6 weeks after birth. Therefore, women who develop PE at high altitude are at greater risk of PAH before and long after birth. Hence, women with a history of PE at high altitude have an increased cardiovascular risk that transcends the systemic circulation to include the pulmonary vascular bed.
How cultural factors along with mental health diagnoses influence the treatment of a stroke patient with no previous mental health history: a case report
- P. Setién Preciados, E. Arroyo Sánchez, A. Sanz Giancola, I. Romero Gerechter, M. Martín Velasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S822-S823
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mental health awareness campaigns in the past few years have vastly improved how medical professionals treat mental health patients. However, prejudices and ignorance still interfere in medical practice. In this context, with the case presented we can see that even in presumed mental health diagnoses along with cultural factors (race, language…), the best medical assistance is not ensured.
ObjectivesReview how different intersectional factors can determine the treatment patients receive at hospitals.
MethodsPresentation of a patient’s case and review of existing literature, in regards to the influence of race, language barriers and mental health diagnoses when attending patients.
ResultsThe patient is presumed to suffer from a mental health condition after a battery of initial tests with inconclusive results do not demonstrate an organic origin. Instead of continuing with the medical study, the patient is disregarded as psychiatric even though his profile doesn´t fit beforehand of a fictitious or conversion disorder. The fact that there are also cultural factors in play (race and language) probably unconsciously influence how the medical team treats this patient’s case. Cultural social factors persistently present as barriers in clinical practice.
ConclusionsRace, language barriers and mental health diagnoses as well as other intersectional factors do have a great impact in the treatment patients receive. There is yet a lot to do when it comes to educating health professionals if we want to offer the best medical assistance.
Disclosure of InterestNone Declared
Suicide behaviour after hospitalisation and related factors: a case report.
- P. Setién Preciados, A. Sanz Giancola, E. Arroyo Sánchez, M. Martín Velasco, I. Romero Gerechter
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1115
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide is a global epidemic, with the World Health Organization (WHO) estimating that there are roughly 800,000 suicides annually, accounting for 1.4% of all deaths, and making suicide the 18th leading cause of death in 2016 (World Health Organization. There is a pressing need to better understand factors that contribute to suicide risk. One important domain for suicide prevention is inpatient psychiatric treatment, as many patients are admitted precisely in order to reduce their risk of suicide. Although inpatient psychiatric treatment is often used for suicide risk prevention the risk of suicide after inpatient treatment remains high. Patients who have been recently discharged have a greater risk of suicide than non-hospitalised mentally ill people.
ObjectivesReview suicidal risk after hospitalisations and the factors that may have an influence on it.
MethodsPresentation of a patient’s case and review of existing literature, in regards to the rate of suicide after a patient is released from psychiatric hospitalisation and the factors that surround it.
ResultsThe patient in question is admitted into a psychiatric ward with a diagnosis of severe psychotic depression, after a suicide attempt trying to dissect his arms’ blood vessels. Health professionals at the hospital attend to his needs and the patient sees improvement. Not long after his release, there is a second hospital admission, which doesn’t have the same result and after his release he successfully ends his life. What comes to mind with these sorts of patients is: what kind of help would they have needed? Why hospital admission was not enough? And which factors and profile of patient is more prone to develop suicide behaviour?
ConclusionsAdmissions at psychiatric wards always have to be thought of as a beneficial resource for patients. There are some cases in which patients do not get the help they need by being hospitalised, increasing the risk of comitting suicide. A lot more studies will have to be carried out to understand what variables play a part in this. Meanwhile an improvement in outpatient care to support patients after hospital release is crucial.
Disclosure of InterestNone Declared
New-Onset Bipolar Disorder in Late Life: a case report and review of literature
- A. Sanz Giancola, E. Arroyo Sánchez, P. Setién Preciados, M. Martín Velasco, I. Romero Gerechter, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S691
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The elderly represents the fastest growing group of the population. It is fair to assume that the portion of old age patients suffering from bipolar disorder will grow in a similar manner. Elderly patients represent approximately 25% of the bipolar population. Summarizing, 5–10% of patients were 50 years of age when they experienced their first manic episode, constituting the subgroup of late onset bipolar disorder (LOBD).
ObjectivesThe purpose of this case report and literature review is to emphasise the importance of LOBD in old population and to highlight its still sparse-knowledge.
MethodsDescriptive case study and review of literature (Arnold,I. et al. Old Age Bipolar Disorder—Epidemiology, Aetiology and Treatment. Medicina 2021,57,587; Baldessarini et al. Onset-age of bipolar disorders at six international sites. J Affect Disord 2010;121(1-2):143-6).
ResultsA 60-year-old woman is brought to the emergency department for evaluation by her family. Over the past 7 days, the patient has become increasingly irritable and argumentative, is sleeping less, is talking faster than usual and has begun to express paranoid concerns about her students “stealing my exam”. The patient is a university professor.
In the assessment interview she is hyperverbal, expansive, and grandiose. The family has also just recently discovered that she has spent a large sum of money on the Internet.
She has no history of psychiatric contact or substance use disorders; however, she has a family history of severe depression.
In the absence of any plausible non-psychiatric condition that could mimic or induce mania, the working diagnosis is bipolar I disorder, most recent episode (MRE) manic with psychotic features.
Image:
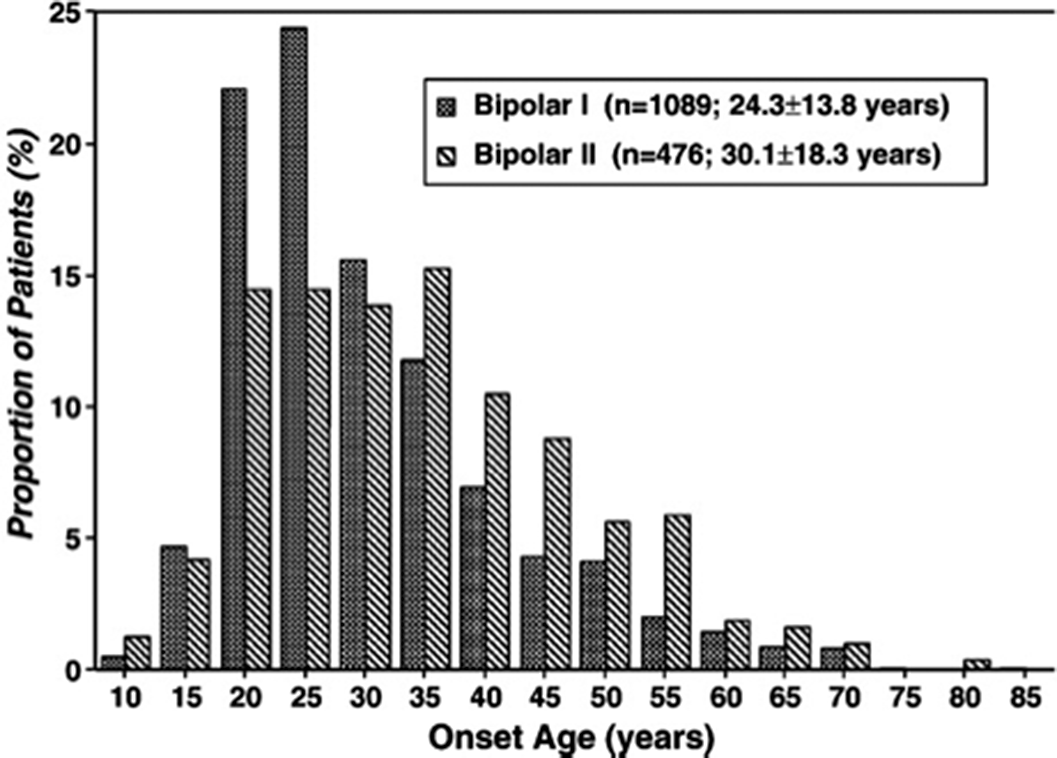
Image 2:
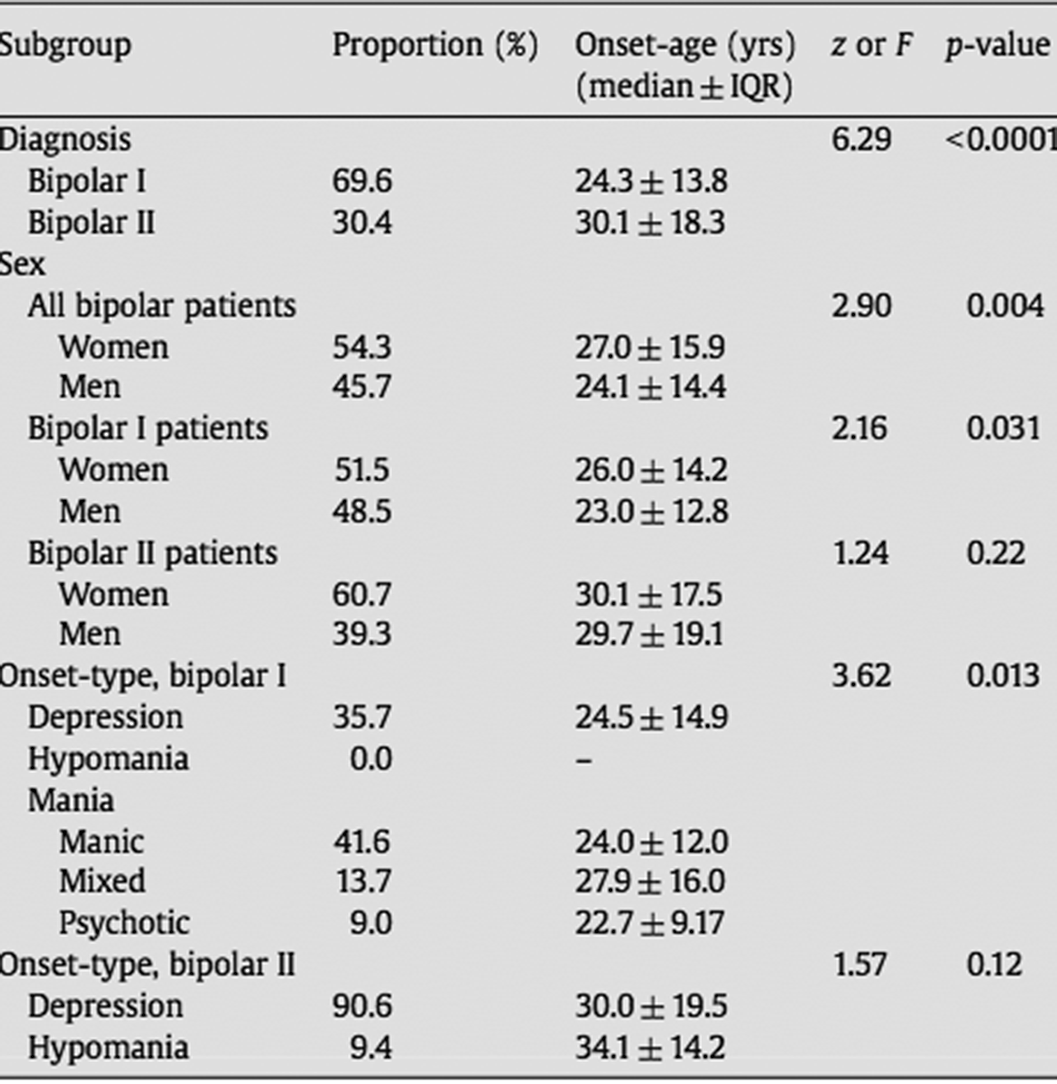 Conclusions
ConclusionsThe share of older age bipolar disorder will grow constantly in the next decades and further research on this neglected patient group is urgently required.
Disclosure of InterestNone Declared
Lithium management in pregnant patients with bipolar disorder
- I. Romero Gerechter, M. Martín Velasco, A. Sanz Giancola, E. Arroyo Sánchez, C. Díaz Mayoral, P. Setien Preciados
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S198
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Women with bipolar disorder often ask their treating clinician for information about family planning, as they are concerned about the impact of their illness on offspring. Pregnancy places additional stress on patients, and physiological changes are particularly acute during postpartum. On the other hand, the risk of abnormalities and teratogenicity from psychotropic drugs is significant. The decision wether resuming or discontinuating lithium is discussed.
ObjectivesWe present a theoretical review on the topic.
MethodsA bibliographic review is presented.
ResultsThe choice to continue medication during pregnancy balances the risks of an untreated illness with the risks of medication exposure. Abrupt discontinuation of psychotropic medications is associated with an increased risk for illness recurrence. Women with BD who discontinue their medications before or during pregnancy have a 71% risk of recurrence with new episodes occurring most frequently in the first trimester. Recurrent illness during pregnancy is associated with a 66% increase in the risk of postpartum episodes. Untreated or under-treated BD during pregnancy is associated with poor birth outcomes independent of pharmacotherapy exposure, including preterm birth, low birth-weight, intrauterine growth retardation, small for gestational age, fetal distress, and adverse neurodeve- lopmental outcomes. Women with untreated BD also have behavioral risk factors such as decreased compliance with prenatal care, poor nutrition, and high-risk behaviors. Impaired capacity to function may result in loss of employment, health care benefits, and social support. The biological and psychosocial risks of a BD episode are the justification for the risk of medication exposure.
Fetal exposure to lithium has been associated with an increased risk for cardiac abnormalities. The risk for Ebstein’s anomaly with first trimester exposure is 1 (0.1%) to 2 in 1000 (0.2%), but the absolute risk remains low. Folate supplementation with 5 mg reduces the risk and severity of congenital heart disease. Lithium toxicity causes lethargy, hypotonia, tachycardia, coma, cyanosis, and chronic twitching in the newborn.
Strategies to minimize fetal exposure and maintain efficacy include using the lowest effective dose, prescribing lithium twice daily to avoid high peak serum concentrations, and regular monitoring of lithium serum concentrations. The effective serum concentration must be established before pregnancy. If a therapeutic concentration has not been established, the lithium dose is titrated to a concentration within the therapeutic range. Breast feeding is discouraged in women taking lithium because of the high rate of transmission to the infant.
ConclusionsTreatment decisions for pregnant women with mood disorders must weigh the potential for increased risks of lithium during pregnancy, especially during the first trimester, against its effectiveness at reducing relapse.
Disclosure of InterestNone Declared
Clozapine use in drug induced psychosis in Parkinson´s disease: a case report and review of literature.
- A. Sanz Giancola, P. Setién Preciados, E. Arroyo Sánchez, I. Romero Gerecther, M. Martín Velasco, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1041
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The occurrence of psychotic symptoms induced by dopaminergic drugs marks a new phase in the course of Parkinson’s disease (PD). The term drug induced psychosis may be used when other significant psychiatric diseases are excluded in patients with no history of psychosis. The prevalence of dopaminomimetic psychosis varies from 5% to 20%. Therefore, knowledge of the psychopharmacological management of this condition is essential.
ObjectivesThe purpose of this case report and literature review is to to learn the psychopharmacological management of this not uncommon medical complication.
MethodsDescriptive case study and review of literature
ResultsWe present the case of a 71-year-old man with a medical history of Parkinson’s disease with partial response to treatment with high doses of levodopa and carbidopa.
He was brought to the emergency department by his family due to the presence of behavioural alterations at home.
The patient reported seeing men in foam trying to harm his family. In a disjointed way in his speech, he links this idea with the delusional belief that he is being watched by electronic devices placed throughout the house. In a variegated manner he links this with a coelotypical type of discourse, however the delusional ideation remains unstructured throughout.
With no previous personal or family history of mental health and ruling out underlying organic conditions, a diagnosis of psychosis secondary to pharmacological treatment for Parkinson’s disease is presumed.
Considering the risks and benefits, it was decided to maintain the anti-Parkinson’s dose in order to avoid worsening the patient’s motor function. Therefore, after reviewing the literature, the best option was to introduce clozapine at low doses, up to 50 mg at night, with the respective analytical control. After a week’s admission, the patient began to improve psychopathologically, achieving an ad integrum resolution of the psychotic symptoms.
ConclusionsDespite the availability of other antipsychotic treatments such as quetiapine or the more recent pimavanserin, clozapine remains the treatment of choice for drug-induced psychosis in Parkinson’s disease.
Disclosure of InterestNone Declared
Clinical management of psychotic pregnancy denial: what do we know? Case report and narrative review.
- M. Martín Velasco, I. Romero Gerechter
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1128-S1129
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Denial of pregnancy is the lack of awareness of being pregnant. It associates with increased morbidity and mortality of mother and child and can be classified as non-psychotic or psychotic. There is few literature regarding the latter, making it difficult to recognize, let alone to treat, since we do not have robust data on the incidence nor approved interventions.
ObjectivesTo get a better understanding on the standard of care for patients with psychotic denial of pregnancy.
MethodsWe present a case report alongside a narrative literature review on the topic.
ResultsWe report the case of a 39-year-old caucasian woman, foreign, undomiciled, who was admitted to a Psychiatry unit due to psychotic symptoms. Her birthplace and prior medical records were unknown. She did not recognize being pregnant and showed great irritability when asked; her responses ranged from delusional attributions of symptoms related to the pregnancy to partially acknowledging her state but refusing to answer questions. Obstetric ultrasound revealed a low risk 35 weeks pregnancy. Treatment included quetiapine up to 700mg daily and psychological approach. A multidisciplinary team managed the case and arranged a plan for delivery. Eventually, delusional symptoms remitted and she accepted the gestation. She showed full collaboration during delivery, giving birth to a healthy female and presented transient recovery. After being separated from her daughter, her clinical situation worsened.
Psychotic denial of pregnancy is rather uncommon. It is usually seen in patients with prior history of major mental illness, most frequently schizophrenia, and important psychosocial vulnerability. It associates with several negative outcomes for mother and baby, including neonaticide. Most studies agree on the need of a multidisciplinary intervention including obstetrics, psychiatry, and others (social agents, ethical consultants…) to generate a plan for mother and baby. Biopsychosocial aspects should always be considered and each case individually formulated. Pregnant women must be given clear and concise information about the process. For some, seeing obstetric ultrasound might help them accept the pregnancy. Some authors propose labour induction prior to 39 weeks and performing a C-section, especially in cases of uncontrolled psychosis or risk of noncompliance. Most studies also recommend antipsychotic treatment. In cases of persistent denial or acute crisis, especially during the third trimester, patients should be admitted to a psychiatry unit with easy access to obstetric care. Supportive psychotherapy and psychosocial intervention should try to identify precipitating stressors for denial, such as prior or anticipated custody loss, which has been linked to psychotic denial.
ConclusionsPsychotic denial is a serious illness which requires a multidisciplinary treatment including biopsychosocial and obstetrical aspects.
Disclosure of InterestNone Declared
Psychotic denial of pregnancy: case report and narrative literature review.
- M. Martín Velasco, I. Romero Gerechter, C. Díaz Mayoral, E. Arroyo Sánchez, A. Sanz Giancola, P. Setién Preciados
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1129
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Denial of pregnancy is the phenomenon where a woman fails to recognize or accept her pregnancy at >20 weeks gestational age. It associates with increased morbidity and mortality of mother and child, and can be classified as non-psychotic or psychotic. There is fewer medical literature regarding the latter, making it difficult to recognize, let alone to treat, since we do not have robust data regarding incidence nor approved interventions or treatment.
ObjectivesTo describe this unfamiliar entity in order to be able to perform a proper diagnosis and thus prevent possible negative outcomes.
MethodsWe present a case report alongside a narrative literature review on the topic.
ResultsWe report the case of a 39-year-old caucasian woman, foreign, undomiciled, with an advanced pregnancy, who was admitted to a Psychiatry in-patient unit due to psychotic symptoms such as mistrust and delusions. She showed scarce collaboration during assessment and did not give any plausible information about her identity. Her birthplace and prior medical records were therefore unknown. Apparently, she had no family nor social support network. Despite the obvious signs, she did not recognize being pregnant and showed great irritability when asked; her responses ranged from claiming she was suffering from a gastric tumor and making delusional attributions of symptoms clearly related to the pregnancy to partially acknowledging her state but refusing to answer any questions on the matter. Blood work showed no significant abnormalities and obstetric ultrasound revealed a low risk 35 weeks pregnancy.
With an estimated prevalence of 1:475 in general population, denial of pregnancy is not as rare as it may seem. The psychotic variant, however, is rather uncommon. Typically, women with psychotic pregnancy denial have prior history of major mental illness, most frequently schizophrenia, and suffer from extreme psychosocial vulnerability. They usually present previous or anticipated child custody loss, which hampers the process of developing antenatal attachment behaviours. Psychotic denial does not associate with concealing, since these women are mentally detached from the gestation and tend to create delusional explanations to their pregnancy symptoms. Not all of them show complete denial, some being able to acknowledge it, though mostly in an inconsistent way. These patients often fail to seek prenatal care or are noncompliant, they are at greater risk of drug exposure, and some are unable to recognize symptoms of labour, all of which increases the rate of negative outcomes for mother and baby, including neonaticide.
ConclusionsPsychotic denial is a rare diagnosis which should be properly assessed due to its clinical implications and the need to prevent potential negative outcomes for mother and baby.
Disclosure of InterestNone Declared
Application of family therapy in a case of anorexia nervosa
- C. Díaz Mayoral, I. Romero Gerechter, E. Arroyo Sánchez, M. Martín Velasco, A. Sanz Giancola, M. Martín de Argila
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S848
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Anorexia nervosa is a behavioral mental disorder, characterized by body dysmorphia, an intense fear of gaining weight and behaviors that interfere with this, in addition to a restriction of food intake, associated usually with medical complications, even a considerable risk of death.
Several psychotherapeutic approaches have been used along last decades. Until relatively recently, parents have been recognized as part of the problem, but nowadays we involve them into the therapeutic process through family therapy based on a systemic approach, recommended in current published clinical guidelines and research findings, with consistent evidence, as the first-line treatment of patients with anorexia nervosa.
ObjectivesA case of a patient with anorexia nervosa, is presented followed by a theoretical review on the topic.
MethodsA case is presented with a bibliographic review.
ResultsA 24-yeard-old female was hospitalized for renutrition due to a significant weight loss and multiple physical symptoms. After 4 months without progress, the patient was transferred to the psychiatric ward.
Once there, physical stabilisation was achieved with family therapy and pharmacological treatment, based on progressive administration of Clomipramine, previously assessed by Cardiology, which improved rumination and obsessive behaviour. We conduct daily individual and weekly family interviews, working on family dynamics, emotional regulation strategies and more adaptive ways of communication. Likewise, several lines of action were found in the systemic work: peripheral father; maternal over-involvement; fraternal rivalry; difficulties of interaction between all of them, derived from “the role of the sick person” and intra-family communication around the illness. Finally, showed effectiveness in terms of an improvement in interpersonal relationships, greater assertiveness and an optimistic attitude with an active search for coping strategies.
ConclusionsHistorically, parents have been recognized by a causal factor in the pathogenesis of this disorder. Nevertheless, the abolition of the emphasis on family responsibility, motivated by a philosophic and evidence-based, has allowed us to see them as an essential resource in aiding the patient in the improvement process. This parental involvement has resulted in a relevant reduction in morbidity, as well as a significant decrease treatment attrition rates. It has been noted a re-establishment in other individual and family factors such as self-esteem, quality of life, and some aspects of the experiences of caregiving, and behavioral symptoms have been resolved.
Disclosure of InterestNone Declared
Relationship between CAINS negative symptoms and cognition, psychosocial functioning and quality of life in patients with a first psychotic episode of schizophrenia
- R. Rodriguez-Jimenez, L. García-Fernández, V. Romero-Ferreiro, M. Valtueña García, A. I. Aparicio, J. M. Espejo-Saavedra, L. Sánchez-Pastor, A. Nuñez-Doyle, M. Dompablo, O. Jiménez-Rodríguez, D. Rentero, P. Fernández-Sotos, I. Martínez-Gras, J. L. Santos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S641-S642
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Negative symptoms has been classically associated with cognition, psychosocial functioning and quality of life in patients with schizophrenia. But negative symptoms are not a unitary construct, encompassing two different factors: diminished expression, and motivation and pleasure. Few works have studied the relationship between these two different negative symptoms factors and cognition (neuro and social cognition), psychosocial functioning and quality of life, jointly, in patients with a first psychotic episode of schizophrenia.
ObjectivesThe objective of the present work was to study, in a sample of patients with a first psychotic episode of schizophrenia, the relationship between the negative symptoms (diminished expression and motivation and pleasure) and neurocognition, social cognition, functioning and quality of life.
MethodsThe study was carried out with 82 outpatients with a first psychotic episode of schizophrenia from two Spanish hospitals (“12 de Octubre” University Hospital, Madrid and “Virgen de la Luz” Hospital, Cuenca). The patients were assessed with the Clinical Assessment Interview for Negative Symptoms (CAINS) for evaluating diminished expression (EXP) and motivation and pleasure (MAP) symptoms, the MATRICS Consensus Cognitive Battery (MCCB) for evaluating neurocognition and social cognition, the Social and Occupational Functioning Assessment Scale (SOFAS), and the Quality of Life Scale (QLS).
ResultsA negative correlation was found between neurocognition and the two negative symptoms subscales: CAINS-EXP (r=-0.458, p<0.001) and CAINS-MAP (r=-0.374, p<0.001); but with social cognition only CAINS-EXP was correlated (r=-0.236, p=0.033). Also, it was found a high negative correlation between SOFAS scores and CAINS-MAP (r=-0.717, p<0.001); and a medium negative correlation with CAINS-EXP (r=-0.394, p<0.001). Finally, QLS score was high correlated with both CAINS subscales: CAINS-EXP (r=-0.681, p<0.001) and CAINS-MAP (r=-0.770, p<0.001).
ConclusionsThis study found a relationship between negative symptoms and neurocognition, social cognition, functioning and quality of life in a sample of patients with a first psychotic episode of schizophrenia. But the two different negative symptom factors, diminished expression, and motivation and pleasure, are associated differently with psychosocial functioning, but especially with social cognition where the relationship was only found with diminished expression symptoms.
Disclosure of InterestNone Declared
PALIPERIDONE PALMITATE 6-MONTH FORMULATION FOR THE TREATMENT OF SCHIZOPHRENIA: A 4-MONTH FOLLOW-UP STUDY
- S. L. Romero Guillena, G. Rodriguez Menendez, A. I. Florido Puerto, A. S. Fernández Flores
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1086-S1087
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Relapse prevention is critical because psychopathology and functionality can worsen in patients with schizophrenia because the repeated episodes and we have strong evidence of antipsychotics efficacy for relapse prevention, but nonadherence rates in patients with schizophrenia are very high, even in comparison with other illness. The literature speaks of average rates of 42% in schizophrenia. For that, long-acting injectable antipsychotics (LAIs) are considered important treatment option, but they are underutilized (Taipale et al. Schizophrenia Bulletin 2017; 44, 1381–1387) (Garcia et al. J Clin Psychopharmacol 2016; 36(4)355-371).
There is extensive clinical trial evidence for the use of paliperidone palmitate 1-month (PP1M) and paliperidone palmitate 3-month (PP3M) formulations for maintaining treatment continuity and preventing relapses and risk of hospitalizations in patients with schizophrenia. (Najarian et al. Int J Neuropsychopharmacol 2022; 25(3) 238-251).
Paliperidone palmitate 6-month (PP6M) formulation is a presentation that provides a dosing interval of once every six months. It is the first and only antipsychotic to be administered twice a year.
ObjectivesThe principal aim of this study was to evaluate the effectiveness, safety, and tolerability of the PP6M in people with non-acute schizophrenia in a naturalistic psychiatric outpatient setting
MethodsSample: 22 patients diagnosed with schizophrenia (DSM 5 criteria) that started treatment with PP6M after being stabilized with PP1M (N:10) or PP3M (N:12) (the treatment dose was not changed in the four months before study inclusion)
The mean dose of PP6M was 822.727 mg
Bimonthly, the following evaluations were performed during a follow-up period of 4 months:
The Clinical Global Impression-Schizophrenia scale (CGI-SCH)
Treatment adherence, concomitant medication, adverse events and the number of hospitalizations and emergency visits
Efficacy values: Percentage of patients who remained free of admissions at the end of 4months of follow-up.
Other evaluation criteria: Percentage of patients who never visited the emergency department at the end of 4 months of follow-up, average change from baseline visit to the final evaluation as assessed by score obtained on the following scale: GSI-SCH, treatment adherence rate and tolerability.
ResultsThe percentage of patients who remained free of admissions at the end of the 4 months was 100% and the percentage of patients who never visited the emergency department at the end of 4 months was 100 %
Mean variations from baseline scores at 4 months were: (-0.21 ±0.31) on the GCI-SCH.
The rate of adherence to treatment with PP6M after 4 months was 100%.
Tolerability was good. None of the patients experienced an adverse event.
ConclusionsIn our study, we found that short-term treatment with paliperidone palmitate 6-month formulation is effective and well tolerated in clinical practice conditions
Disclosure of InterestNone Declared
Mania induced after corticosteroid treatment: a case report
- E. Arroyo Sánchez, A. Sanz- Giancola, P. Setién Preciados, I. Romero Gerechter, M. Martín Velasco, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S697
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Corticosteroids are drugs widely used in clinical practice for their anti-inflammatory and immunosuppressive properties. Despite their beneficial effects, a high association of these drugs with neuropsychiatric adverse effects such as psychosis, mania, depression, delirium or increased risk of suicide, among others, has been observed. We present the case of 54-year-old man who started treatment with hydroaltesone 20 mg/8h after undergoing surgery for a pituitary macroadenoma who began with maniform clinic.
ObjectivesTo know the prevalence, risk factors and treatment of mania as a side effect of corticosteroid drugs.
MethodsPresentation of the case and review of the available literature on the risk of developing mania after corticosteroid treatment.
ResultsSeveral studies confirm that the incidence of psychiatric adverse effects after the use of corticosteroids is around 6% if we refer to severe reactions; 28% moderate reactions; and 72% if we consider milder reactions. The direct relationship between these drugs and affective symptoms ranges in rates between 1-50% of cases, the most frequent being depression and mania. The risk of mania after treatment with corticosteroids is 4-5 times higher than if we compare it with a group of population not exposed to these drugs. There is a dose-response relationship, increasing the risk from a daily dose of 40 mg/day, with an average duration of symptoms of around 21 days. Female sex seems to be a risk factor in relation to the fact that diseases requiring this type of treatment are more common in this gender. As first-line treatment for mania secondary to corticosteroids, a decrease in treatment dose or its interruption, whenever possible, is proposed. Adjuvant treatment may be required, with atypical antipsychotics being the first choice.
ConclusionsCorticosteroid therapy has a direct dose-response relationship with the presence of psychiatric adverse effects such as mania. Dose and sex have been studied as possible adverse effects. Therefore, the pharmacological treatment of choice consists of a reduction in the dose of corticosteroids administered or withdrawal, if possible, and may be combined with an atypical antipsychotic such as olanzapine, quetiapine or risperidone. Re-evaluation is recommended until complete resolution of the clinical picture and then antipsychotic treatment can be progressively withdrawn.
Disclosure of InterestNone Declared
Cremations and Pyrotechnologies among the Prehispanic Inhabitants of Cerro de Trincheras, Northern Mexico
- Jessica I. Cerezo-Román, Thomas R. Fenn, Carlos Cruz Guzmán, Silvia I. Nava Maldonado, Claudia León Romero, Elisa Villalpando
-
- Journal:
- Latin American Antiquity / Volume 34 / Issue 1 / March 2023
- Published online by Cambridge University Press:
- 09 November 2022, pp. 1-20
- Print publication:
- March 2023
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Using data from several well-preserved pyres, which are rarely found well preserved in the southwestern United States and northern Mexico, we examine cremation customs and their associated pyrotechnologies at the site of Cerro de Trincheras in northern Sonora, Mexico, from AD 1300 to 1450/1500. We explore variations in pyre construction and use, thermal alterations of the deceased, the deceased individuals’ biological profiles, the performance of mortuary rituals, and the sensorial experiences of both the mourners and the wider Cerro de Trincheras community. The residents of the site were masters of the pyrotechnologies associated with cremations, making efficient pyres for the deceased and maximizing their resources. The group also created transformative funeral rituals that may have facilitated and mediated a wide range of emotional responses toward their deceased.
Reinforcing the new diagnosis of Complex Post-Traumatic Stress disorder (CPTSD) of ICD-11: exploring the clinical outcomes in youth exposed to complex trauma
- L. Marques Feixa, S. Romero, J. Moya-Higueras, P. Santamarina-Pérez, J. March-Llanes, M.J. Muñoz, I. Zorrilla, M. Rapado-Castro, H. Blasco-Fontecilla, E. Anglada, M. Ramirez, L. Fañanas
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S448-S449
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Youth exposed to complex trauma (CT) show an increased risk of psychiatric morbidity, including a wide range of psychiatric disorders. However, to date, there is no specific diagnosis in the DSM-5 that capture the clinical complexity of these patients. Properly, the last version of the ICD-11 includes a diagnosis termed Complex Post-Traumatic Stress Disorder (CPTSD), which considers the pattern of post-traumatic stress symptoms, plus life-impairing disturbances in self-organization (emotion dysregulation, negative self-concept and interpersonal problems). Clinical research about CPTSD, especially in younger population, is still limited.
ObjectivesTo explore the symptomatology of CPTSD in a sample of youth exposed to CT and its association with worse clinical outcomes.
Methods187 youth aged 7 to 17 years participated in the EPI_young_stress_project (116 with current psychiatric disorder and 71 healthy controls). CT was evaluated following the TASSCV criteria. To identify CPTSD symptomatology, we performed an exploratory factor analysis including CBCL and TEIQue items. The global level of functioning was measured by CGAS.
ResultsPreliminary results pointed that youth exposed to CT showed greater internalizing (p<.001) and externalizing (p<.001) symptomatology. Regardless of their current primary diagnosis based on DSM-5, youth exposed to CT reported more CPTSD symptomatology (p<.001). Moreover, youth with CPTSD showed greater use of psychotropic drugs (p<.001), higher and longer hospitalizations (p=.002) and worse overall functioning (p<.001).
ConclusionsThe inclusion of the CPTSD in future versions of mental disorders manuals should increase the implementation of early specific trauma interventions, which may improve victims’ lives and reduce the risk of worse clinical outcomes.
DisclosureNo significant relationships.
Children and adolescents exposed to maltreatment already exhibit epigenetic patterns suggestive of heightened low-grade inflammation
- H. Palma-Gudiel, L. Marques Feixa, S. Romero, M. Rapado-Castro, H. Blasco-Fontecilla, I. Zorrilla, M. Martín, Á. Castro Quintas, J.L. Monteserin-Garcia, E. Font, M. Ramirez, D. Moreno, M. Marín-Vila, N. Moreno, E. Binder, L. Fañanas
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S71
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Childhood maltreatment (CM) is one of the best described environmental risk factors for developing any psychiatric disorder, while it also confers increased odds for obesity, cardiometabolic disorders and all-cause mortality. Inflammation has been suggested to mediate the widespread clinical effects of CM. Previously, Ligthart et al. (2016) identified a polyepigenetic signature of circulating CRP levels, a measure of chronic low-grade inflammation, that has been reliably associated with a wide array of complex disorders. The study of this biomarker could dilucidate the mechanistic relationship between CM and psychiatric outcomes.
ObjectivesThus, CRP-associated epigenetic modifications were explored regarding proximal exposure to CM.
MethodsGenomic DNA was extracted from peripheral blood mononuclear cells of 157 children and adolescents (7 to 17 years old). Exposure to CM was assessed following the TASSCV criteria. Genome-wide DNA methylation was assessed by means of the EPIC array. Fifty-two out of the 58 original CRP-associated CpG sites surpassed quality control and were included in the analysis. Age, sex, psychopathological status and cell type proportions were included as covariates.
ResultsDNA methylation at 12 out of 52 CpG sites (23%) was significantly associated with exposure to CM (p < .05); 8 of these associations survived correction for multiple testing (q < .05).
ConclusionsThis is the first study to date to explore the relationship between childhood maltreatment and an epigenetic signature of chronic low-grade inflammation. Our findings underscore the presence of immune dysregulation early after exposure to CM; further studies are needed to assess the long-term clinical implications of this signature in psychiatric patients.
DisclosureNo significant relationships.
Prevalence and covid 19 vaccination rate in a population of patients with schizophrenia and a substance use disorder
- S.L. Romero Guillena, I. De Burgos Berdud, R. Gálvez Medina, E. Serrano Rodriguez
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S267
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
As of August 27th, 2021, the diagnosed cases of COVID 19 in Spain are 4 758 003 with a prevalence of 10.03%. 68.4% of the Spanish population is fully vaccinated
ObjectivesPrimary: To compare the prevalence of COVID infection in a cohort of patients with schizophrenia to patients with a dual diagnosis of schizophrenia and substance use disorder Secondary: To compare the rate of fully vaccinated patients diagnosed with schizophrenia with and without a coexisting substance use disorder.
MethodsRetrospective descriptive study. The population in study is made up of patients with schizophrenia (46) and dual diagnosis schizophrenia (28) (following DSM 5 criteria) Confirmed cases were those cases with positive PCR
ResultsThere was not a stadistically significant difference in the prevalence of COVID 19 infection between both groups of patients. The prevalence of COVID infection among the dual diagnosis schizophrenia was 3.57% compared to 6.5% in those without coexisting substance abuse disorder. Relative to vaccination rate, we didn’t find a stadistically significant difference between both groups. However, there was a higher vaccination rate in the dual diagnosis schizophrenia group (82.12%) compared to the non-dual diagnosis schizophrenia group (69.56%)
ConclusionsThe prevalence of COVID 19 infection in the dual diagnosis schizophrenia cohort is 3.57% and in the group of patients with schizophrenia without substance abuse disorder is 6,5%. In those with dual diagnosis schizophrenia the vaccination rate was un 82.12%. It was 69.56% in those without coexisting substance abuse disorder.
DisclosureNo significant relationships.
Griefing reaction and social networks
- M.D.C. Molina Liétor, M. Martín, I. Cuevas Iñiguez, I. Romero Gerechter, A. Sanz Giancola
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S577
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Grief is a normal and not necessarily pathological psychological process that occurs after the loss of a family member or loved one with its psycho-affective consequences, external manifestations and rituals. Although mourning processes can be associated with losses of different types (employment, housing, baseline situation, housing), we will refer to mourning for the loss of a loved one. For some people, social networks facilitate the expression of feelings and experiences of grief, connecting with the emotional support of other friends and loved ones. However, the presence of accounts belonging to these deceased persons, the persistence of photos and memories that periodically appear on the screen without the person being able to choose them, can make it difficult to process the mourning.
ObjectivesThe aim of this paper is to consider the beneficial and detrimental factors of social media during a grieving reaction after the loss of a loved one.
MethodsFor the preparation of this work, a bibliographic review on the subject has been carried out. Likewise, the clinical information provided by patients during our evaluations has provided critical views on what has been published in this regard.
ResultsSupport through social networks can help to feel more affectionate, but there are other harmful factors that must be taken into account: permanence of photos, appearance of memories and reminder of the deceased person’s birthday.
ConclusionsSocial networks can have favorable but also detrimental factors in the elaboration of a grief and should be considered in the psychiatric exploration and intervention.
DisclosureNo significant relationships.
Neurosyphilis as a cause for neuropsychiatric symptoms: a case report
- I. Romero Gerechter, M.D.C. Molina Liétor
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S656
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Syphilis is a sexually transmitted infection which in its late phase can cause all kinds of neuropsychiatric symptoms. A case report of a 79-year-old male with a manic episode probably due to lues is presented.
ObjectivesA case of a patient with neurosyphilis is presented followed by a theoretical review on the topic.
MethodsA case is presented with a bibliographic review.
ResultsA 79-year-old male was hospitalized with symptoms of disorientation, inattention, and difficulty for abstract thought. His speech was verbose, incoherent with megalomaniac ideas. He presented affective symptoms such as hyperthymia, emotional lability and intermittent crying. He also had nomination problems and recent memory mistakes. He also suffered from insomnia. He presented as his medical history HIV infection under control and syphilis treated in December 2020 with a negative RPR test in June 2021. During his hospitalization he was treated with increasing doses of olanzapine and valproic acid. Irritability improved with this treatment.
ConclusionsNeurosyphilis may be presented as any kind of neuropsychiatric disorder. Laboratory tests are required as there is no conclusive imaging test. Penicillin and symptomatic management are the proper treatment. Neuropsychiatric disorders in elderly population must consider infectious diseases and previous pathologies as differential diagnosis.
DisclosureNo significant relationships.
Prevalence and correlates of suicidal behaviour in adolescents with bipolar disorder
- S. Romero, I. Mendez, S. Lera, P. Santamarina
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S28-S29
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Objective
To examine the prevalence and correlates of suicidal behavior among adolescents with bipolar disorder (BD).
Methods47 adolescents, ages 12 to 19 years (15.8 ± 2), meeting DSM-5 criteria for BD-I (n=40) and BD-II (n=7) were assessed using the KSADS-PL and tested with a battery of tests measuring mood, psychotic symptoms, life events and functioning. History of suicidal attempts (SA) was ascertained using the K-SADS-PL.Results: One third (n=15, 32%) of the BD sample had a lifetime history of SA. There were no differences in socio-demographics factors between SA versus non- SA. BD adolescents with lifetime SA, were more likely to have lower weight at birth, a lifetime history of comorbid eating disorder, non-suicidal self-injurious behavior, 2nd degree family history of suicide attempt, and more stressful life events as compared with non-attempters. Adolescents with lifetime history of SA also showed statistically significant higher scores in depression, suicidal ideation and anxiety as compared with BD adolescents without lifetime SA. Logistic regression analysis found that the most robust correlates of SA in adolescents with BD were having 2nd degree family history of SA, the interaction of self-injury behavior and comorbid eating disorder and increased number of life events. Limitations: Retrospective data. Small sample size. Since this is a cross-sectional study, no inferences regarding causality can be made. Conclusion: One third of the adolescents with BD have attempted suicide. These results are in agreement with previous studies. History of SA in adolescents with BD is strongly associated with family history of suicidal behavior, lifetime self-injury behavior with comorbid eating disorder and increased number of stressful life events.
DisclosureNo significant relationships.
Ten new insights in climate science 2020 – a horizon scan
- Erik Pihl, Eva Alfredsson, Magnus Bengtsson, Kathryn J. Bowen, Vanesa Cástan Broto, Kuei Tien Chou, Helen Cleugh, Kristie Ebi, Clea M. Edwards, Eleanor Fisher, Pierre Friedlingstein, Alex Godoy-Faúndez, Mukesh Gupta, Alexandra R. Harrington, Katie Hayes, Bronwyn M. Hayward, Sophie R. Hebden, Thomas Hickmann, Gustaf Hugelius, Tatiana Ilyina, Robert B. Jackson, Trevor F. Keenan, Ria A. Lambino, Sebastian Leuzinger, Mikael Malmaeus, Robert I. McDonald, Celia McMichael, Clark A. Miller, Matteo Muratori, Nidhi Nagabhatla, Harini Nagendra, Cristian Passarello, Josep Penuelas, Julia Pongratz, Johan Rockström, Patricia Romero-Lankao, Joyashree Roy, Adam A. Scaife, Peter Schlosser, Edward Schuur, Michelle Scobie, Steven C. Sherwood, Giles B. Sioen, Jakob Skovgaard, Edgardo A. Sobenes Obregon, Sebastian Sonntag, Joachim H. Spangenberg, Otto Spijkers, Leena Srivastava, Detlef B. Stammer, Pedro H. C. Torres, Merritt R. Turetsky, Anna M. Ukkola, Detlef P. van Vuuren, Christina Voigt, Chadia Wannous, Mark D. Zelinka
-
- Journal:
- Global Sustainability / Volume 4 / 2021
- Published online by Cambridge University Press:
- 27 January 2021, e5
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Non-technical summary
We summarize some of the past year's most important findings within climate change-related research. New research has improved our understanding of Earth's sensitivity to carbon dioxide, finds that permafrost thaw could release more carbon emissions than expected and that the uptake of carbon in tropical ecosystems is weakening. Adverse impacts on human society include increasing water shortages and impacts on mental health. Options for solutions emerge from rethinking economic models, rights-based litigation, strengthened governance systems and a new social contract. The disruption caused by COVID-19 could be seized as an opportunity for positive change, directing economic stimulus towards sustainable investments.
Technical summaryA synthesis is made of ten fields within climate science where there have been significant advances since mid-2019, through an expert elicitation process with broad disciplinary scope. Findings include: (1) a better understanding of equilibrium climate sensitivity; (2) abrupt thaw as an accelerator of carbon release from permafrost; (3) changes to global and regional land carbon sinks; (4) impacts of climate change on water crises, including equity perspectives; (5) adverse effects on mental health from climate change; (6) immediate effects on climate of the COVID-19 pandemic and requirements for recovery packages to deliver on the Paris Agreement; (7) suggested long-term changes to governance and a social contract to address climate change, learning from the current pandemic, (8) updated positive cost–benefit ratio and new perspectives on the potential for green growth in the short- and long-term perspective; (9) urban electrification as a strategy to move towards low-carbon energy systems and (10) rights-based litigation as an increasingly important method to address climate change, with recent clarifications on the legal standing and representation of future generations.
Social media summaryStronger permafrost thaw, COVID-19 effects and growing mental health impacts among highlights of latest climate science.





